World News
Moderate Hypofractionation in Breast Cancer Treatment: A Safe and Effective Approach
1. Understanding Hypofractionation: A Shift in Radiation Therapy
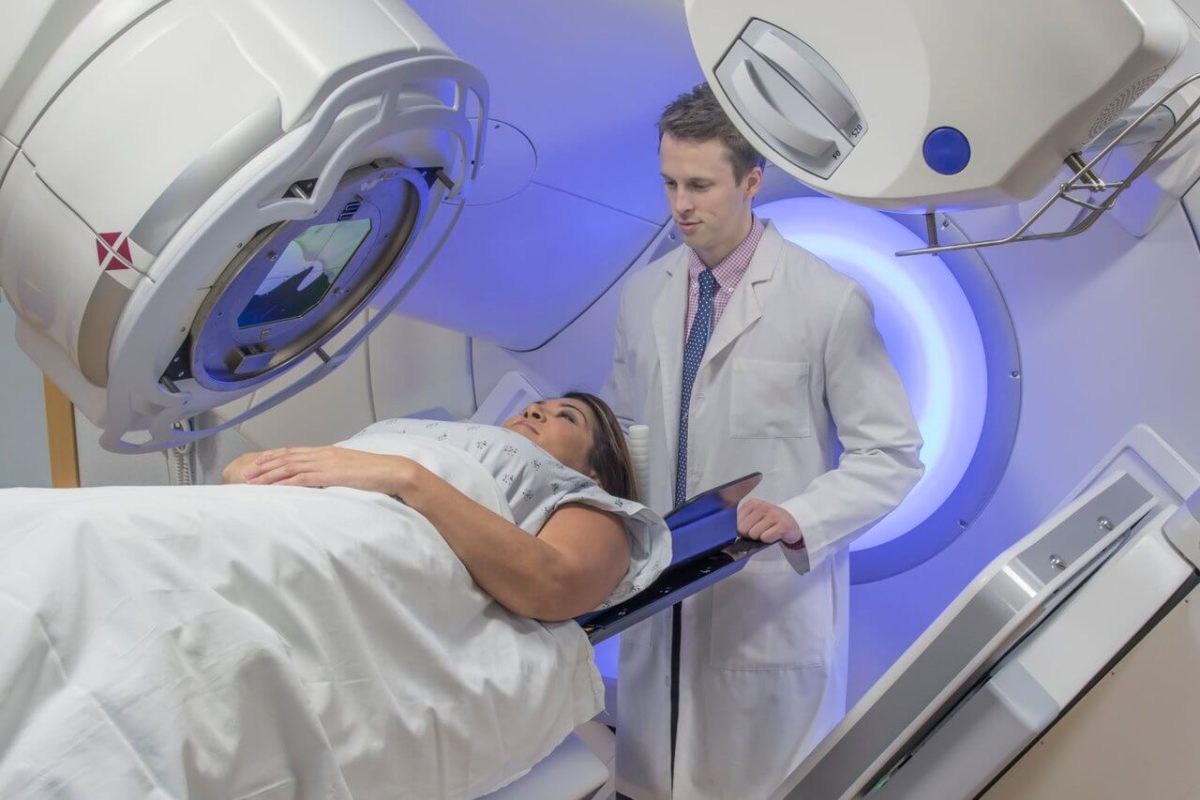
Radiation therapy has long been a cornerstone in the treatment of breast cancer, helping to reduce recurrence rates and eliminate cancer cells that may remain after surgery. Traditionally, radiation therapy involves delivering smaller doses over an extended period, often requiring patients to undergo treatment for several weeks. However, a growing body of research has shown that hypofractionation, a method where larger doses of radiation are administered over a shorter time span, can be just as effective while offering additional benefits. Moderate hypofractionation, in particular, has emerged as a promising approach for patients with early-stage breast cancer. This technique allows for fewer treatment sessions without compromising efficacy, making it a more convenient option for patients. In recent years, studies have highlighted the safety and effectiveness of this method, suggesting that moderate hypofractionation may soon become a new standard of care in breast cancer treatment.
2. The Safety and Efficacy of Moderate Hypofractionation
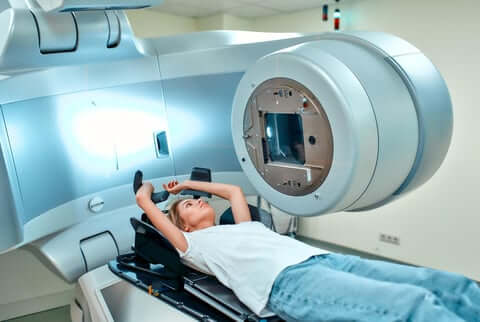
One of the key concerns when introducing a new radiation therapy approach is its safety profile. Fortunately, multiple studies have demonstrated that moderate hypofractionation is not only safe but also highly effective in treating breast cancer. Research has shown that this approach yields similar long-term outcomes to conventional radiation therapy, with no significant increase in the risk of complications or damage to surrounding healthy tissues. In fact, moderate hypofractionation has been associated with favorable side effect profiles, including fewer skin reactions and less fatigue. These positive safety outcomes have been particularly reassuring for patients who may be concerned about the potential risks of undergoing more intensive radiation treatments. Moreover, the ability to complete treatment in a shorter timeframe has significant implications for patient quality of life, reducing the emotional and physical toll often associated with prolonged therapy. As more studies continue to confirm the safety and efficacy of moderate hypofractionation, its adoption is expected to grow in clinical practice.
3. Convenience and Quality of Life: Benefits for Patients
One of the most significant advantages of moderate hypofractionation is its potential to improve the overall experience for breast cancer patients. Traditional radiation therapy often requires daily visits to the treatment center for several weeks, which can be physically and emotionally exhausting. For patients balancing work, family responsibilities, and the stress of a cancer diagnosis, the length of treatment can be a major burden. Moderate hypofractionation, by reducing the number of sessions required, offers a more convenient and manageable alternative. Patients can complete their radiation therapy in a fraction of the time, allowing them to return to their normal routines sooner. This approach also reduces the need for frequent travel to treatment centers, particularly benefiting those who live in rural areas or far from specialized facilities. The improvement in convenience and quality of life has made moderate hypofractionation an attractive option for both patients and healthcare providers, especially as cancer care increasingly focuses on patient-centered approaches.
4. Expanding Access to Care Through Hypofractionation
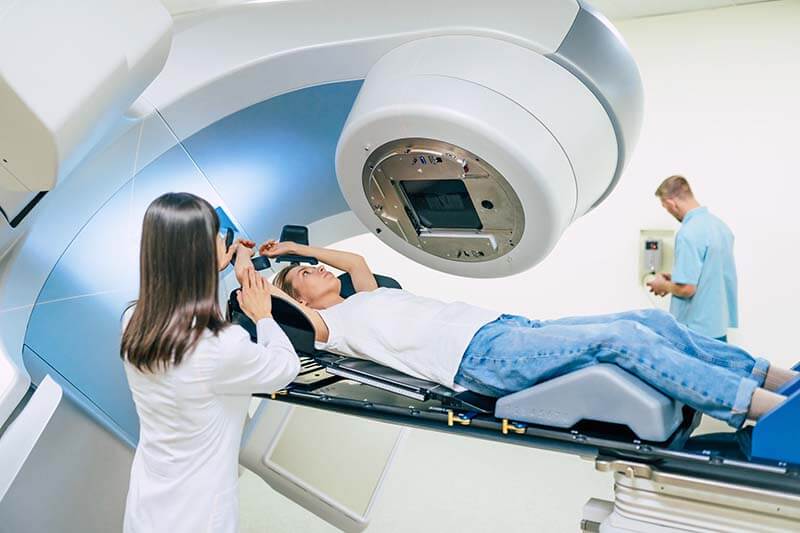
Another critical benefit of moderate hypofractionation is its potential to expand access to care, particularly for underserved populations. Radiation therapy can be a resource-intensive treatment, often requiring specialized equipment and personnel. In many regions, especially in low-resource settings or rural areas, access to radiation therapy can be limited due to logistical challenges. By reducing the number of required sessions, moderate hypofractionation can help ease the burden on healthcare facilities and make treatment more accessible to a wider range of patients. This shorter treatment course also helps reduce costs for both patients and healthcare systems, making it a more cost-effective option. As healthcare providers seek ways to improve accessibility and reduce disparities in breast cancer treatment, moderate hypofractionation presents a viable solution that can help bridge the gap in care. Its ability to deliver high-quality treatment in a shorter time frame offers significant advantages in ensuring that more patients receive timely and effective cancer care.
5. The Future of Breast Cancer Radiation Therapy: Moving Toward a New Standard
As research on moderate hypofractionation continues to evolve, it is becoming clear that this approach holds great promise for the future of breast cancer radiation therapy. With its demonstrated safety, efficacy, and potential to improve patient quality of life, moderate hypofractionation is poised to become a new standard of care for early-stage breast cancer patients. Ongoing clinical trials are exploring its use in more complex cases, including patients with larger tumors or those requiring more extensive radiation fields. As the medical community continues to embrace this approach, guidelines are being updated to reflect its benefits, and more patients are being offered this treatment as an option. The shift toward moderate hypofractionation also reflects a broader trend in oncology, where treatments are becoming increasingly personalized and tailored to meet the specific needs and preferences of patients. As we move forward, moderate hypofractionation represents an important step in improving breast cancer care, offering a safer, more efficient, and patient-centered approach to radiation therapy.
From Ecomhao